Endometrial Thickness in Assisted Reproduction
The relevance of the endometrial thickness in assisted reproduction is progressively gaining momentum. This is dedicated to the outline of “all the intended parents have to know” concerning the human endometrium. While physicians understood a long time ago that both a viable embryo along with a receptive uterus were needed for successful embryo implantation, much of the focus since that has been on improving embryo viability as opposed to the endometrial thickness. Therefore, Parents Life informs and encourages the intended parents to carry on pushing the limitations of the endometrial thickness.
The endometrial thickness is especially true for the female reproductive tract and particularly the endometrium, where there are unpredictable responses to hormonal therapies, along with other factors that lead to poor reproductive along with other health outcomes. We hope that the intended parents are motivated to think about the complexities of the human endometrium in clinical practice and women’s well-being as well as in research in order to advance women’s reproductive health beyond empirical therapies, unpredictable endometrial responses and unpredictable prognoses for contraception, fertility treatments, pregnancy outcomes and endometrial morbidities.
A normally functioning endometrium is important for reproductive success and the well-being of women. In its multiple roles, including quality control for embryo implantation and pregnancy, an enormous energy commitment for a long gestation, orderly development, and synchronized processes leading to tissue homeostasis, and as a sentinel for upper reproductive tract infections, it is important to think about this tissue as a master regulator of reproductive performance and women’s health. It was recommended that ecosystem, ovarian function and age are likely to be the major determinants of the endometrial thickness variation, function and reproductive success. Therefore, what is the role of genetics, epigenetics, metabolomics, the microbiomes of the gut and reproductive tract, along with other omics in endometrial responsiveness to ovarian hormones and separate from ovarian hormones?
Parents Life posit these could be elucidated with deep phenotyping clinically and large data from large numbers of women over the life span and around the globe. Indeed, modern medicine holds great promise to optimize women’s reproductive health more broadly soon for current and future generations.
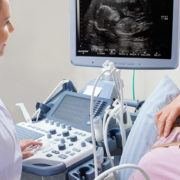
Transvaginal ultrasound is a technique for initial evaluation of the endometrial echo texture and thickness in women presenting with pre- and post- menopausal uterine bleeding and infertility patients undergoing ovulation monitoring. Saline infusion sonohysterography (SIS) and 3D ultrasound are sensitive diagnostic modalities for the detection of endometrial polyps, intrauterine adhesions, submucous or intracavitary leiomyoma and hereditary uterine anomalies, highly similar to MRI and hysteroscopy. The 3D ultrasound enables detailed assessment of the endometrium and vascularization, while increasing the diagnostic precision of ultrasound in the evaluation of endometrial lesions.










Leave a Reply
Want to join the discussion?Feel free to contribute!